To ease your shift to a hospital bed, focus on creating a comfortable, accessible space by organizing essentials within reach and adding safety features like grab bars. Practice safe techniques for getting in and out of bed, and use supportive pillows and devices to make moving easier. Communicate your needs clearly with caregivers, stay active with gentle exercises, and maintain a positive outlook. Keep exploring to discover more helpful tips for a smoother transition.
Key Takeaways
- Communicate openly with caregivers about comfort needs, positioning, and emotional concerns to ensure proper support.
- Use proper positioning techniques, pillows, and supports to promote comfort and prevent pressure sores.
- Shift positions at least every two hours and perform gentle exercises to reduce stiffness and improve circulation.
- Create a safe, accessible room layout with grab bars, good lighting, and essential items within reach.
- Practice mindfulness, engage in enjoyable activities, and seek emotional support to ease emotional adjustment.
Why Transitioning to a Hospital Bed Can Be Challenging: And How to Make It Easier

Adjusting to a hospital bed can be difficult because it often represents a significant change in your daily routine and environment. Emotional adjustment is a major hurdle, as you may feel frustration, sadness, or anxiety about your new situation. These feelings can be overwhelming, but family support plays a vital role in easing the transition. Having loved ones nearby provides reassurance and helps you feel less isolated. Sharing your concerns and listening to theirs creates a sense of connection and understanding. Remember, it’s normal to struggle initially. Lean on your family for encouragement, and don’t hesitate to express your feelings. Additionally, understanding the importance of emotional adjustment strategies can help you cope better during this time. Incorporating innovative European cloud servers into your healthcare management can also facilitate better communication with caregivers and access to support resources. Recognizing the value of effective communication can significantly ease the process. Developing coping skills and finding comfort in familiar routines can further support your emotional well-being. Building emotional resilience and embracing small daily successes can make the adjustment smoother. With time, emotional adjustment becomes easier, especially when you’re supported by those who care about your well-being.
Creating a Comfortable, Accessible Space for Your Hospital Bed
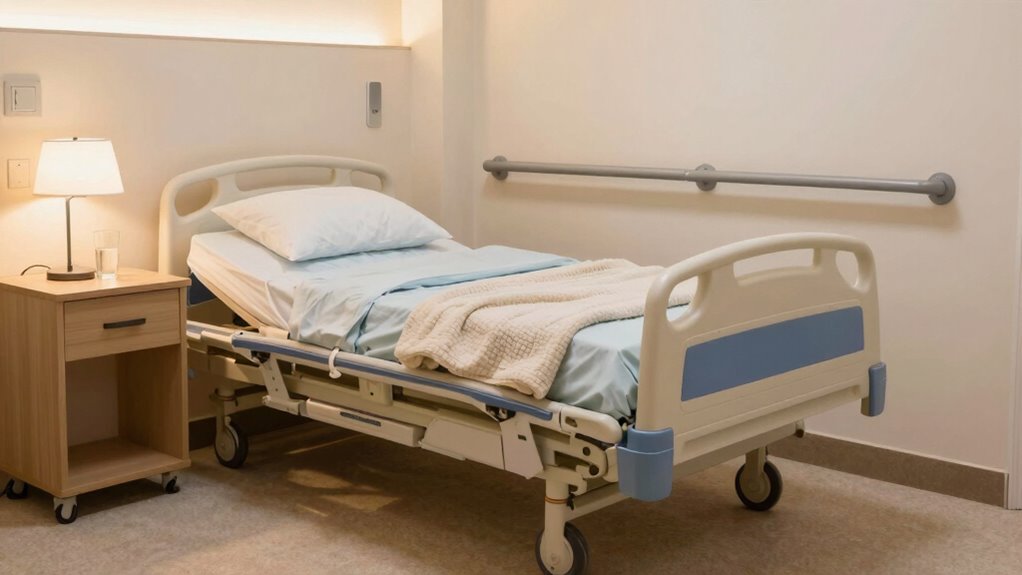
To make your hospital bed feel more comfortable and accessible, start by optimizing the room layout to allow easy movement around it. Adding safety features like grab bars and non-slip mats can prevent falls and boost your confidence. Taking these steps helps create a space that’s both functional and reassuring. Remember to stay aware of your surroundings and make smart choices to promote your safety. Incorporating room organization strategies can further enhance the flexibility and adaptability of your space, making it easier to adjust as your needs change. Additionally, integrating smart technology can help monitor your environment and provide assistance when needed, increasing your independence. Ensuring proper lighting in the room can also significantly reduce fall risk and improve visibility.
Optimize Room Layout
Creating a comfortable and accessible space for your hospital bed starts with thoughtful room layout. Proper space organization and furniture placement guarantee safety and ease of movement. To achieve this, consider these key points:
- Position the bed near a wall or corner to maximize open space and reduce clutter.
- Arrange furniture so pathways are clear, ideally a minimum of 3 feet wide, for easy navigation.
- Keep essential items like a nightstand and call button within arm’s reach, avoiding obstructed access.
- Incorporate safe positioning techniques to further enhance comfort and prevent injuries during movement and transfers. Utilizing proper room layout principles can help optimize space and promote safer patient mobility.
- Pay attention to space-saving techniques to ensure the room remains functional and comfortable for both the patient and caregivers.
Enhance Safety Features
Enhancing safety features around your hospital bed is essential to prevent falls and accidents. During the adjustment period, you’ll need to pay close attention to safety awareness to identify potential hazards. Install sturdy handrails and ensure the bed’s wheels lock securely when in use. Keep the area clear of clutter and loose rugs that could cause tripping. Adequate lighting is vital, especially at night, to help you navigate safely. Consider adding a bed alarm if needed for extra security. Regularly check that safety features are functioning properly and adjust them as necessary. When choosing accessories, opt for high-quality safety equipment to ensure maximum protection. Additionally, understanding wiring basics can help you troubleshoot and maintain electrical components safely. Being familiar with hospital bed mechanisms can also aid in proper operation and prevent malfunctions. Educating yourself about proper bed positioning can further enhance safety and comfort during use. By actively improving safety measures, you create a secure environment that promotes confidence and reduces risk during your transition to a hospital bed.
Learn Safe Techniques for Getting In and Out of Bed

Getting in and out of bed safely is essential to prevent falls and injuries, especially when adjusting to a hospital bed. Proper bed mobility and safe transfer techniques help you maintain stability. To further enhance safety, consider integrating smart home technology such as motion sensors or voice-controlled devices to assist with mobility and alerts. Additionally, practicing safe transfer techniques regularly can build confidence and improve your overall safety during movement. Improving your understanding of bed mobility principles can also contribute to safer transfers. Here’s how to do it:
- Sit on the edge of the bed with your feet flat on the floor, supporting your weight with your hands if needed.
- Use your arm strength and leg muscles to lean back slowly, then swing your legs over the side of the bed.
- When standing, keep your back straight and use your legs to rise, avoiding twisting or sudden movements.
- Remember to maintain proper body alignment throughout the transfer to reduce strain and support balance. Proper body positioning is especially important when adapting to specialized beds to ensure safety and comfort.
Using Supportive Pillows and Devices to Make Moving Safer and Easier

Using supportive pillows and devices can substantially improve your safety and comfort when moving in and around your hospital bed. Supportive pillows help maintain proper alignment, reducing strain on your joints and muscles during transfers. Positioning devices, such as bed rails or transfer aids, provide stability and leverage, making movements smoother and safer. Place supportive pillows behind your back or between your knees to prevent sliding or discomfort. Use positioning devices to assist with turning or sitting up, minimizing the risk of falls or injuries. These tools work together to make repositioning easier, giving you more control and confidence. Incorporating vacuum-assisted tools such as bed rails and transfer aids can further enhance your stability and reduce the risk of accidents during transfers. Always verify pillows and devices are correctly positioned and secure before moving, to maximize safety and comfort during your transition. Additionally, understanding the importance of proper equipment setup can help optimize their effectiveness and ensure your safety during movements.
How to Position Yourself for Comfort and Safety
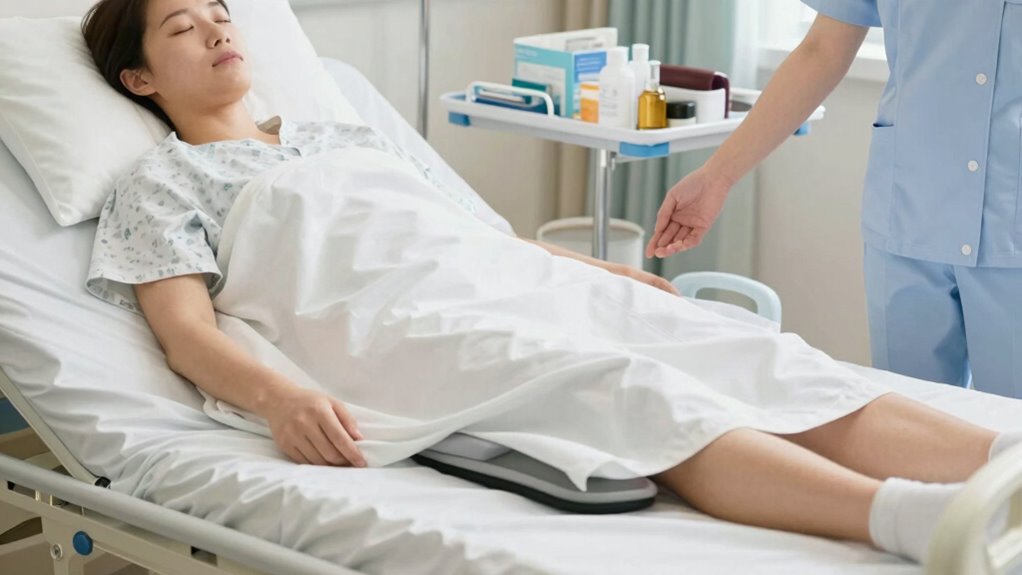
Proper positioning in your hospital bed helps you stay comfortable and safe during movement. To achieve this, focus on ergonomic positioning and cushion placement. First, adjust your bed so your body aligns naturally, supporting your back and neck. Second, position cushions strategically: place lumbar supports to maintain proper spinal alignment and use pillows to elevate limbs as needed. Third, assure your hips and knees are slightly bent when sitting up, reducing strain. Proper cushion placement prevents discomfort and promotes stability, making transfers easier and safer. Always check that your body is well-supported and avoid positions that cause pain or strain. Small adjustments in positioning can considerably improve your comfort and safety during your hospital stay.
Prevent and Manage Pressure Sores and Muscle Stiffness
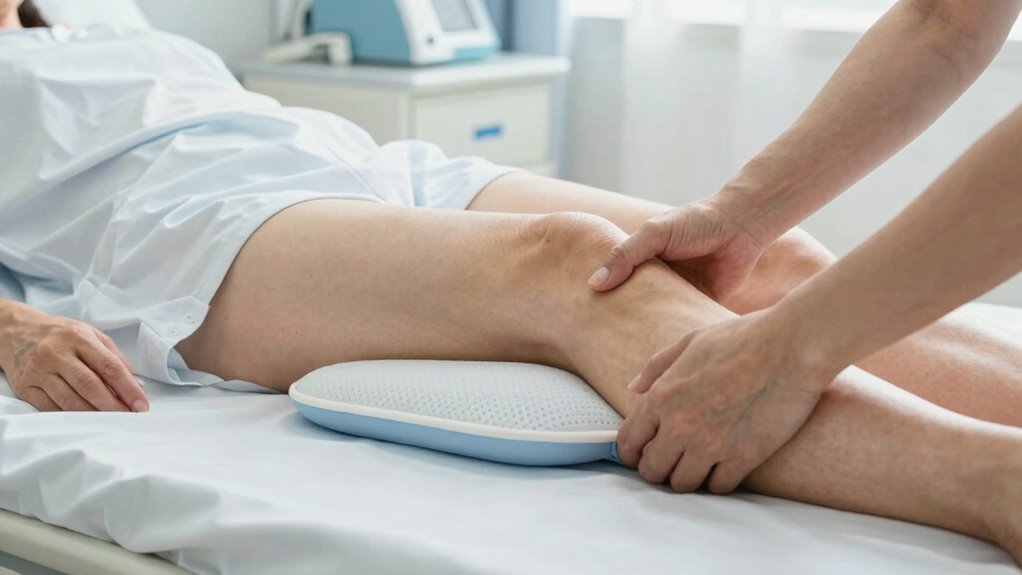
To prevent pressure sores and muscle stiffness, maintaining regular position changes and keeping your skin clean and dry is vital. Effective pressure management involves shifting your position at least every two hours to reduce pressure on vulnerable areas. Use pillows or cushions to offload weight from bony prominences and support proper alignment. Skin protection is essential; inspect your skin daily for signs of redness or breakdown, especially in areas prone to pressure. Keep your skin clean and moisturized to prevent dryness and irritation. Proper hygiene helps avoid infections and promotes skin health. Staying mobile within your limits, performing gentle exercises if possible, also aids in reducing stiffness. Consistent pressure management and vigilant skin protection are key to preventing complications and ensuring your comfort.
Communicating Your Needs Clearly With Caregivers and Staff

To guarantee your needs are understood, use clear and simple language when talking with caregivers and staff. Make certain to confirm they understand your preferences and concerns regularly. Sharing specific care instructions helps everyone provide the best support during your transition.
Use Clear, Simple Language
Clear communication is essential when explaining your needs to caregivers and staff. Using simple language helps guarantee they understand your specific concerns about bed mobility and emotional adjustment. Be direct and specific about what you need, such as assistance with turning in bed or adjusting your position comfortably. Here are three ways to do this effectively:
- Use clear, straightforward instructions like “Help me turn to the left” instead of vague phrases.
- Mention specific feelings or worries, such as anxiety about physical changes or emotional adjustment.
- Confirm that caregivers understand your needs by asking them to repeat instructions or clarify any doubts.
Confirm Understanding Regularly
Since misunderstandings can lead to frustration or even accidents, it’s important to check in regularly with caregivers and staff to make certain they truly understand your needs. Clear caregiver communication ensures your bed positioning is correct and that your comfort is maintained. Ask questions like, “Is my head elevated properly?” or “Can you adjust the bed for better support?” Use this table to guide your conversations:
| Question to Ask | What to Confirm | Why It Matters |
|---|---|---|
| Is my bed positioned correctly? | Proper alignment and safety | Prevents strain or falls |
| Are my comfort needs understood? | Adjustments for pain relief | Ensures comfort and safety |
| Do you understand my mobility limits? | Safe transfer techniques | Reduces injury risk |
Regular check-ins help you stay in control of your care.
Share Specific Care Preferences
Sharing your specific care preferences helps guarantee caregivers and staff understand exactly what you need to stay comfortable and safe. Clear bedside communication is essential for reducing confusion and easing your emotional adjustment to the hospital bed. To make sure your needs are met, consider sharing:
- Your preferred position and how often you’d like to change it
- Any specific pain management routines or comfort measures
- Your emotional support needs, like familiar objects or quiet time
Doing Gentle Exercises to Improve Circulation and Flexibility

Gentle exercises can especially boost circulation and flexibility, making your shift to a hospital bed more comfortable. Start with simple gentle stretching to loosen tight muscles and improve blood flow. Focus on movements that target your arms, legs, and neck, avoiding any pain or discomfort. Incorporate mobility exercises, such as ankle circles or leg lifts, to maintain joint flexibility and prevent stiffness. These exercises help prevent blood clots and reduce muscle atrophy, which are common concerns during periods of limited mobility. Perform your exercises slowly and intentionally, breathing steadily throughout. Doing these regularly can make your transition easier and support your overall comfort and recovery. Always check with your healthcare provider before starting any new exercise routine to guarantee safety.
Staying Positive During Your Hospital Bed Transition

Staying positive can make a big difference as you adjust to your hospital bed. Focus on engaging in activities that lift your spirits and keep you connected with loved ones. A positive outlook helps you stay motivated and find hope during this shift.
Maintaining a Positive Outlook
Maintaining a positive outlook can significantly influence your recovery and overall well-being during the shift to a hospital bed. Embracing mindset shifts helps you view challenges as opportunities for growth, fostering emotional resilience. To stay optimistic:
- Focus on small daily achievements to build confidence.
- Practice gratitude by recognizing what’s going well each day.
- Surround yourself with encouraging words and supportive people.
These actions reinforce your ability to adapt and maintain a hopeful perspective. Your mindset directly impacts your healing process, making it easier to cope with emotional ups and downs. Remember, staying positive isn’t about ignoring difficulties but rather cultivating resilience to face them head-on, boosting your chances of a smoother transition and quicker recovery.
Engaging in Supportive Activities
Engaging in supportive activities can play a pivotal role in keeping your spirits high during the shift to a hospital bed. Creative activities like drawing, journaling, or listening to music can boost your mood and give you a sense of accomplishment. These activities provide emotional support by helping you express feelings and process your experiences. Staying connected with loved ones through calls or virtual visits offers reassurance and comfort. Additionally, practicing mindfulness or meditation can reduce stress and foster a positive outlook. By focusing on supportive activities, you empower yourself to stay engaged and hopeful, making the transition easier and more manageable. Remember, small acts of positivity can greatly impact your emotional well-being during this challenging time.
When to Seek Help for Difficulties or Concerns

Recognizing when to seek help is essential during your shift to a hospital bed, especially if you notice persistent discomfort, confusion, or difficulty managing daily tasks. Emotional adjustment can be challenging, and caregiver communication helps identify when concerns are urgent. Watch for these signs:
- You feel overwhelmed or anxious despite efforts to adapt.
- You experience ongoing confusion, memory issues, or difficulty understanding instructions.
- Tasks like bathing, eating, or mobility become consistently difficult or unsafe.
If any of these occur, don’t hesitate to reach out. Prompt support can improve emotional well-being and ensure safety. Remember, seeking help isn’t a sign of weakness—it’s a crucial step in managing your transition and addressing concerns early.
Frequently Asked Questions
How Can I Maintain My Independence While Using a Hospital Bed?
You can maintain your personal independence by practicing bedside mobility exercises and adjusting the bed to your comfort. Use grab bars and assistive devices to move safely, and stay engaged in small tasks to keep your skills sharp. Communicate your needs with caregivers, and take an active role in your daily routines. This approach helps preserve your autonomy while ensuring safety and comfort during your stay.
Are There Specific Mattress Types That Reduce Pressure Sores?
Yes, you should consider pressure relief mattresses to reduce pressure sores. Foam mattress types are especially effective because they evenly distribute your weight and minimize pressure points. These mattresses adapt to your body’s shape, providing better comfort and reducing the risk of sores. Talk to your healthcare provider about the best foam or specialty pressure relief mattress for your needs, ensuring you stay comfortable and protected while in your hospital bed.
What Are Common Signs of Discomfort or Complications to Watch For?
You should watch for signs like persistent pain, redness, swelling, or changes in skin color, which can indicate bedsores prevention issues. Also, be alert to new discomfort, difficulty moving, or numbness, signaling mobility challenges or complications. If you notice these signs, act quickly—adjust positions, seek medical advice, or notify caregivers—to prevent further issues and promote comfort during your hospital stay.
How Do I Adapt My Daily Routine After Transitioning to a Hospital Bed?
After shifting to a hospital bed, you should adapt your routine by prioritizing bedside mobility exercises to prevent stiffness and improve circulation. Adjust your sleep position regularly to find the most comfortable and supportive posture, reducing discomfort and pressure points. Incorporate short walks if possible, and set reminders for repositioning throughout the day. These steps help you stay comfortable and promote healing during your recovery.
Can Family Members Be Trained to Assist With Bed-Related Tasks?
Yes, family members can be trained to assist with bed-related tasks. For example, you might teach a family member proper bed assistance techniques, like safe repositioning or helping with transfers. Family training guarantees they understand safety protocols and can provide effective support, fostering independence and reducing caregiver stress. This approach makes daily care more manageable and promotes a comfortable environment for your loved one.
Conclusion
Remember, moving to a hospital bed is like steering a gentle river—you may hit gentle rapids, but with patience and support, you’ll flow smoothly. Embrace each step as part of your journey toward comfort and recovery. Keep communication open and use the tools and techniques that work best for you. Soon, this new chapter will feel more like a steady, peaceful stream, guiding you toward renewed strength and restful days ahead.









