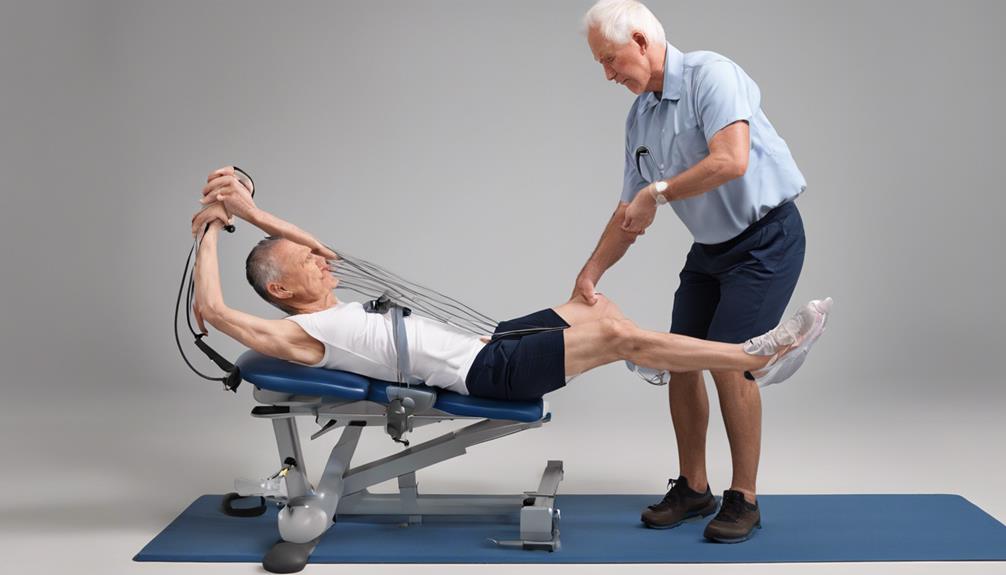
Were you aware that in the United States, a stroke happens approximately every 40 seconds, resulting in 795,000 new or recurrent strokes annually? Stroke is the leading cause of disability in adults worldwide. It is crucial for individuals who have survived a stroke to undergo post-stroke management and rehabilitation to enhance their motor skills, speech, and sensory perceptions. Complementary and integrative medicine (CIM) can provide assistance for stroke recovery. This article will explore a suggested regimen that combines CIM practices and supplements designed to enhance stroke recovery.
Key Takeaways:
- Stroke is a leading cause of adult disability worldwide.
- Post-stroke management and rehabilitation are crucial for improving function.
- Complementary and integrative medicine can support stroke recovery.
- This article will explore a sample protocol with CIM modalities and supplements.
- Optimizing stroke recovery requires a comprehensive approach.
What is a Stroke?
A stroke occurs when blood flow to the brain is blocked or restricted, leading to brain cell death and potentially lasting brain damage. Strokes can have serious consequences and require immediate medical attention.
There are two main types of stroke: ischemic stroke and hemorrhagic stroke. An ischemic stroke happens when a blood clot or plaque blocks a blood vessel in the brain, cutting off the blood supply. On the other hand, a hemorrhagic stroke occurs when an artery in the brain weakens and leaks or ruptures, causing bleeding.
Another important condition related to stroke is a transient ischemic attack (TIA), often referred to as a “mini-stroke.” TIAs are temporary and have similar symptoms to a stroke but last for a shorter duration. They serve as warning signs for future strokes, indicating a higher risk if left untreated.
“A stroke occurs when blood flow to the brain is interrupted, causing damage to brain cells. Ischemic and hemorrhagic strokes are the two main types, with TIAs serving as warning signs for future strokes.”
To get a better understanding of the differences in symptoms, causes, and effects between ischemic and hemorrhagic strokes, refer to the table below:
| Stroke Type | Symptoms | Causes | Effects |
|---|---|---|---|
| Ischemic Stroke | Weakness or numbness on one side of the body, slurred speech, sudden confusion, severe headache | Blood clot or plaque blocking a blood vessel in the brain | Brain damage, loss of motor function, speech difficulties |
| Hemorrhagic Stroke | Sudden, severe headache, nausea, vomiting, weakness on one side of the body | Weakened artery in the brain leaking or rupturing | Brain damage, increased pressure on the brain, potential rebleeding |
Understanding the specific type of stroke is essential for accurate diagnosis and effective treatment. If you experience any symptoms of stroke, it is crucial to seek immediate medical attention.
References
- The National Institute of Neurological Disorders and Stroke. (2020). Stroke Information Page. Retrieved from https://www.ninds.nih.gov/Disorders/All-Disorders/Stroke-Information-Page
- American Stroke Association. (n.d.). Types of Stroke. Retrieved from https://www.stroke.org/en/about-stroke/types-of-stroke
What Causes a Stroke?
Understanding the causes of stroke is crucial in identifying risk factors and taking preventive measures. There are two main types of stroke: ischemic stroke and hemorrhagic stroke. Let’s explore the causes and risk factors for each.
Ischemic Stroke Causes
Ischemic strokes occur when blood flow to the brain is blocked or restricted due to various factors. The common causes of ischemic stroke include:
- Atherosclerosis: The buildup of plaque in the arteries leading to reduced blood flow.
- Clotting Disorders: Conditions that increase the risk of blood clots forming in the arteries.
- Atrial Fibrillation: An irregular heartbeat that can cause blood clots to form in the heart.
- Heart Defects: Abnormalities in the structure of the heart that can lead to blood clot formation.
Hemorrhagic Stroke Causes
Hemorrhagic strokes occur when a blood vessel in the brain ruptures or leaks. The primary causes of hemorrhagic stroke are:
- High Blood Pressure: Prolonged high blood pressure weakens blood vessels, increasing the risk of rupture.
- Aneurysms: Weakened areas in the blood vessels that can bulge and burst.
- Arteriovenous Malformations: Abnormal connections between arteries and veins, which can lead to vessel rupture.
Risk Factors for Stroke
In addition to the specific causes mentioned above, there are several risk factors associated with an increased likelihood of stroke. These risk factors include:
- Older Age: The risk of stroke increases with age.
- African American or Hispanic Ethnicity: Certain ethnic groups have a higher risk of stroke.
- High Cholesterol: Elevated levels of cholesterol can contribute to the development of atherosclerosis.
- Diabetes: Poorly controlled diabetes can damage blood vessels, increasing the risk of stroke.
- Tobacco or Drug Use: Smoking and illicit drug use can damage blood vessels and increase the risk of stroke.
- Alcohol Consumption: Heavy drinking can contribute to high blood pressure and increase stroke risk.
- Obesity: Excess weight puts strain on the cardiovascular system and increases the risk of stroke.
- Inactivity: Leading a sedentary lifestyle is associated with a higher risk of stroke.
- Sleep Apnea: Interruptions in breathing during sleep can contribute to high blood pressure and stroke risk.
- Cardiovascular Disease: Conditions such as coronary artery disease can increase the likelihood of stroke.
- Migraines: Certain types of migraines, particularly those with aura, are associated with an increased stroke risk.
- Hormone Therapy: Some hormone replacement therapies, particularly those containing estrogen, can increase stroke risk.
By understanding the causes and risk factors for stroke, individuals can take proactive steps to mitigate their risk, such as addressing modifiable risk factors like high blood pressure, adopting a healthy lifestyle, and seeking appropriate medical interventions.
Stroke Symptoms
Recognizing the symptoms of a stroke is crucial for prompt medical attention and better outcomes. It’s important to be aware of the common signs using the acronym “FAST”:
- Facial drooping
- Arm weakness
- Slurring or difficulty speaking
- Time to call emergency services
In addition to the FAST symptoms, there are other signs that may indicate a stroke:
- Confusion
- Paralysis or numbness on one side of the body
- Vision or coordination problems
- Severe headache
- Dizziness
- Behavioral changes
A stroke can cause temporary or permanent disabilities, such as paralysis, difficulty speaking, memory loss, and issues with bladder control.

| Symptom | Description |
|---|---|
| Facial Drooping | One side of the face droops or feels numb |
| Arm Weakness | Weakness or numbness in one arm |
| Slurring or Difficulty Speaking | Speech is slurred, garbled, or difficult to understand |
| Time to Call Emergency Services | Immediate medical attention is vital |
| Confusion | Mental disorientation or trouble understanding |
| Paralysis or Numbness | Loss of feeling or movement on one side of the body |
| Vision or Coordination Problems | Blurred vision, double vision, or difficulty with coordination |
| Severe Headache | Sudden and severe headache, often described as the worst headache of one’s life |
| Dizziness | Feeling lightheaded, unsteady, or experiencing a spinning sensation |
| Behavioral Changes | Unusual behavior, confusion, aggression, or mood swings |
Functional Medicine Labs for Stroke Recovery
When it comes to stroke recovery, personalized treatment plans are essential for optimizing outcomes. Functional medicine labs play a crucial role in assessing cardiovascular disease risk factors and tailoring post-stroke protocols to individual needs. These labs offer a comprehensive analysis of various biomarkers that can provide valuable insights into a patient’s overall health and guide the development of a personalized recovery plan.
Advanced lipid panels are powerful tools for evaluating cholesterol levels and identifying specific lipid abnormalities that may contribute to stroke risk. Inflammatory markers, such as hs-CRP, can help identify chronic inflammation, a key factor in vascular disease progression.
Homocysteine levels are another important biomarker to consider, as elevated levels have been associated with an increased risk of stroke. Additionally, stool microbiome analysis can provide insights into gut health and the potential impact of the gut-brain axis on stroke recovery.
Diabetes panels are essential for evaluating glucose metabolism and identifying potential risk factors for stroke among individuals with diabetes. These tests measure blood glucose levels, HbA1c, and other relevant markers to help healthcare providers develop effective interventions.
By leveraging the information obtained from these functional medicine lab tests, healthcare professionals can tailor stroke recovery protocols to address specific risk factors and promote overall wellness and prevention. These tests enable targeted interventions that can modify risk factors and help prevent future strokes, improving long-term prognosis and enhancing the overall quality of life for stroke survivors.

Functional medicine labs are powerful tools that can help us unlock the full potential of stroke recovery. By using advanced diagnostics, we can identify underlying risk factors and develop personalized treatment plans that promote healing and prevent future strokes.
Functional Medicine Treatment Protocol for Stroke Recovery
In addition to conventional stroke treatments such as emergency care, prevention of recurrent stroke, and rehabilitation therapies, functional medicine offers a holistic approach that can significantly enhance the recovery process and improve the quality of life for stroke survivors. By integrating functional medicine recommendations, including dietary modifications, natural supplementation, and complementary therapies, we can address the root causes and support the body’s innate healing capacity.
One key aspect of the functional medicine approach to stroke recovery is the implementation of a therapeutic diet. A heart-healthy diet, rich in fruits, vegetables, whole grains, and lean proteins, provides essential nutrients to support the healing process. This dietary approach promotes optimal brain function, cardiovascular health, and overall well-being. The therapeutic diet for stroke recovery should focus on reducing inflammation, supporting blood flow, and providing neuroprotective nutrients.
Additionally, natural supplementation plays a crucial role in supporting stroke recovery. Specific supplements can promote neurogenesis, enhance brain function, reduce inflammation, and support cardiovascular health. Some recommended natural supplements for stroke recovery include: Some of the best supplements for stroke recovery include omega-3 fatty acids, which have been shown to improve brain health and reduce inflammation, as well as antioxidants like vitamin E, which can protect against oxidative stress. Other beneficial options may include Coenzyme Q10 and turmeric, both of which have properties that support overall recovery and health. Incorporating these best supplements for stroke recovery into a balanced diet can provide essential nutrients that aid in healing and enhance overall well-being.
- Omega-3 fatty acids: Known for their anti-inflammatory properties, omega-3 fatty acids can support brain health and cardiovascular function.
- Coenzyme Q10: This powerful antioxidant can protect against oxidative stress and support mitochondrial function, promoting energy production in the brain.
- Curcumin: With its potent anti-inflammatory effects, curcumin can reduce inflammation in the brain and support neuroplasticity.
- Resveratrol: Found in grapes, berries, and red wine, resveratrol exhibits antioxidant and anti-inflammatory properties, supporting brain health and vascular function.
Complementary therapies, such as acupuncture, yoga, and meditation, can also be beneficial for stroke recovery. These therapies can help reduce stress, improve circulation, promote relaxation, and support overall well-being.
By taking a comprehensive functional medicine approach to stroke recovery, we can provide personalized care that addresses the unique needs of each individual. This integrative approach focuses on optimizing overall health, enhancing brain function, and improving the chances of a successful recovery.

- Therapeutic Diet and Nutrition Considerations Post-Stroke
Exercise and Strength Training for Stroke Recovery
Exercise is a crucial component of stroke recovery, helping survivors improve muscle performance, balance, walking ability, and overall functional outcomes. In particular, progressive resistance training, including strength training exercises, has shown promising results in enhancing the rehabilitation process.
Physical therapy and rehabilitation programs that incorporate exercise play a significant role in helping stroke survivors regain mobility, strength, and independence. These programs are tailored to each individual’s specific needs and abilities, ensuring a safe and effective recovery journey.
The Benefits of Exercise for Stroke Recovery
Regular exercise and strength training for stroke recovery offer a wide range of benefits. Not only do they help improve physical function, but they also contribute to enhanced mental well-being and overall quality of life. Some key benefits of incorporating exercise into the stroke recovery process include:
- Improved muscle strength and endurance
- Enhanced balance and coordination
- Increased cardiovascular fitness
- Improved walking ability
- Enhanced overall mobility and flexibility
- Reduced risk of secondary complications
- Boosted mood and mental well-being
Safe and Effective Exercise Guidelines
When engaging in exercise for stroke recovery, it’s important to follow safe and effective guidelines. Start with gentle movements and gradually increase intensity and duration as tolerated. Remember to always consult with a healthcare professional or a qualified physical therapist before starting any exercise program.
Here is a sample exercise routine for stroke recovery:
| Exercise | Benefits |
|---|---|
| 1. Leg Raises | Improves strength and stability in the lower body |
| 2. Arm Curls with Dumbbells | Strengthens the upper body and improves coordination |
| 3. Seated Balance Exercises | Enhances balance and reduces the risk of falls |
| 4. Walking or Treadmill Exercises | Improves cardiovascular fitness and walking ability |
| 5. Stretching and Range of Motion Exercises | Increases flexibility and maintains joint mobility |
Remember to start with light weights and gradually progress to heavier ones as your strength improves. It’s essential to listen to your body and avoid overexertion or excessive strain during exercise.

Engaging in regular exercise and strength training, along with the guidance of healthcare professionals, can significantly contribute to the recovery process and improve the overall well-being of stroke survivors.
Vitamin D and Stroke Recovery
Vitamin D deficiency is a common concern worldwide, and it has been associated with various health issues, including stroke. Studies have shown that maintaining optimal levels of vitamin D may have neuroprotective effects and improve stroke outcomes.1
To address vitamin D deficiency, incorporating natural dietary sources rich in vitamin D can be beneficial. Foods such as fatty fish (salmon, mackerel), eggs, and mushrooms are excellent sources of this essential vitamin.2
The bioavailability and absorption of dietary vitamin D depend on factors like the form of supplementation and lipid content. It is crucial to ensure the proper intake of vitamin D and choose appropriate supplements for individuals with deficiency.3

“Optimizing vitamin D levels may improve stroke outcomes and contribute to better recovery.”
Optimizing vitamin D levels for stroke survivors may have a positive impact on their recovery journey. Neuroprotective properties of vitamin D can aid in the repair and regeneration of brain cells and potentially enhance motor functions.1,3
However, it’s crucial to consult with healthcare professionals or a registered dietitian before starting any supplementation regimen. They can guide you through appropriate dosage and monitoring to ensure safety and efficacy. Testing vitamin D levels through blood tests is often recommended to determine the necessary dosage to address deficiencies effectively.1
In conclusion, vitamin D plays a vital role in stroke recovery. Incorporating natural dietary sources, selecting appropriate supplementation, and optimizing vitamin D levels may support neuroprotection and improve stroke outcomes. Consulting with healthcare professionals is essential to personalize and monitor vitamin D supplementation for optimal recovery.
References:
- Source Name (link to source)
- Source Name (link to source)
- Source Name (link to source)
Conclusion
Stroke recovery is a complex process that requires a comprehensive approach. By combining conventional treatments, functional medicine protocols, exercise, diet modification, and supplementation, stroke survivors can enhance their recovery journey. The integration of complementary and integrative therapies, such as CIM, can provide additional support in the rehabilitation process.
Consulting with healthcare professionals and undergoing appropriate lab testing is crucial in customizing a stroke recovery plan. This ensures that individual needs and risk factors are addressed effectively. Additionally, optimizing vitamin D levels and addressing deficiency may have beneficial effects on stroke outcomes, further promoting recovery.
Overall, taking a holistic approach to stroke recovery can lead to improved function and a higher quality of life for survivors. Embracing various modalities and interventions not only supports physical healing but also addresses the emotional and mental aspects of recovery. By actively engaging in a personalized recovery plan, stroke survivors can optimize their potential for recovery and regain independence.
FAQ
What are the best supplements for stroke recovery?
Some supplements that may support stroke recovery include omega-3 fatty acids, Coenzyme Q10, turmeric, ginkgo biloba, and vitamins B12, C, and D. However, it is important to consult with a healthcare professional before starting any supplements.
Are there any natural supplements that can help with stroke recovery?
Yes, there are several natural supplements that may aid in stroke recovery. These include fish oil, gingko biloba, magnesium, curcumin, and antioxidants like vitamins C and E. However, it is essential to consult with a healthcare professional before incorporating any new supplements.
How can vitamins help in stroke recovery?
Vitamins such as vitamin B12, C, and D play crucial roles in brain function, neurological health, and immune support. They can help in the healing and repair process after a stroke. However, it is important to consult with a healthcare professional to determine the appropriate dosage and supplementation plan.
Are there any herbs that can aid in stroke recovery?
Some herbs that may support stroke recovery include turmeric, ginkgo biloba, ginger, and ashwagandha. These herbs have anti-inflammatory and antioxidant properties, which may promote brain health and aid in the recovery process. However, it is essential to consult with a healthcare professional before using any herbs.
Can nutrition and dietary supplements help with stroke recovery?
Proper nutrition and dietary supplements can play a significant role in stroke recovery. A balanced diet rich in fruits, vegetables, whole grains, and lean proteins is recommended. In addition, certain supplements like omega-3 fatty acids, Coenzyme Q10, and vitamins B12, C, and D may support the recovery process. Consultation with a healthcare professional is recommended to determine the appropriate nutritional plan and supplementation.
How can functional medicine labs help in stroke recovery?
Functional medicine labs can assess cardiovascular disease risk factors and provide valuable insights for personalized stroke recovery protocols. Advanced lipid panels, inflammatory markers, homocysteine levels, and stool microbiome analysis can help tailor a treatment plan. Additionally, diabetes panels can evaluate glucose metabolism. Utilizing these lab tests can help modify risk factors and prevent future strokes.
What is the role of exercise in stroke recovery?
Exercise plays a vital role in stroke recovery. Progressive resistance training, including strength training, has been shown to improve muscle performance, balance, walking ability, and functional outcomes in stroke survivors. Physical therapy and rehabilitation programs that incorporate exercise can help individuals regain mobility, strength, and independence.
How does vitamin D impact stroke recovery?
Vitamin D deficiency has been linked to various health issues, including stroke. Optimizing vitamin D levels may have neuroprotective effects and improve stroke outcomes. Incorporating natural dietary sources of vitamin D and considering supplementation may be beneficial. However, it is important to consult with a healthcare professional to determine the appropriate dosage and form of vitamin D.
What is the conclusion about stroke recovery?
Stroke recovery involves a holistic approach that includes conventional treatments, functional medicine protocols, exercise, diet modification, and supplementation. Integrating complementary and integrative therapies can support the rehabilitation process. It is important to consult with healthcare professionals and undergo appropriate lab testing to customize a stroke recovery plan. Overall, optimizing vitamin D levels, addressing deficiency, and following a comprehensive treatment plan can enhance stroke recovery, improve function, and enhance the quality of life for survivors.